Overuse injuries in youth soccer are common, but most are manageable when parents and coaches recognize early warning signs and respect growing bodies. Two of the more common overuse injuries particular to youth soccer players are Osgood-Schlatter and Sever’s Disease. Below is an overview of other injury scenarios you may encounter as a parent – it’s good to be prepared.
Why overuse is a “youth soccer problem”
- Overuse injuries happen when small amounts of stress pile up faster than the body can recover, especially with year-round play, tournaments, and multiple teams.
- Growing athletes are more vulnerable because growth plates are weaker than surrounding bone and tendon, and bones often grow faster than muscles can adapt.
- Research suggests that a sizable portion of youth soccer injuries each season are overuse-related, particularly around the knee and ankle
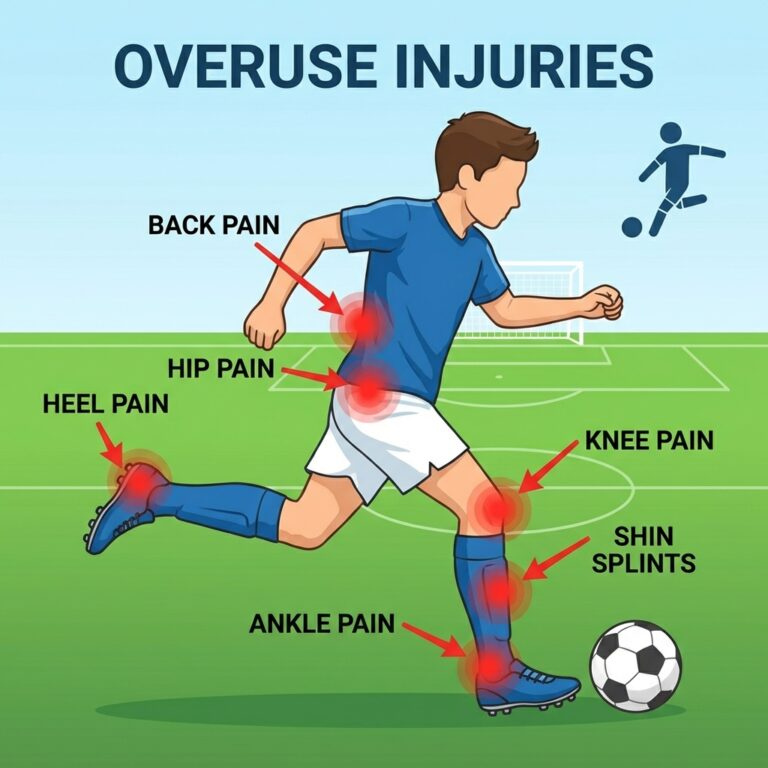
Common overuse injuries in youth soccer
- Knee pain
- Patellofemoral pain (“runner’s knee”): dull, achey pain around or behind the kneecap, worse with stairs, squats, running, or sitting with bent knees.
- Patellar tendinopathy (“jumper’s knee”): pain just below the kneecap, aggravated by repeated jumping, sprinting, or striking the ball.
- Sinding-Larsen-Johansson: growth-plate irritation at the lower tip of the kneecap, often described as Osgood-Schlatter’s “cousin” higher up the chain.
- Hip, pelvis, and lower back
- Hip and pelvic apophysitis: irritation where major muscles attach to the growing pelvis and upper thigh bone, causing groin or front-hip pain with sprinting and kicking.
- Low back pain and spondylolysis: stress-related irritation or small defects in the spine of adolescent athletes who extend or rotate their backs repeatedly.
- Shin, foot, and ankle problems
- Shin splints (medial tibial stress syndrome): exercise-related pain along the inner edge of the shin, common with training spikes or hard surfaces.
- Stress reactions and stress fractures: more focal bone pain that worsens with impact and may linger at rest, often in the shin, foot, or metatarsals.
- Achilles tendinopathy and plantar fasciitis: pain at the back of the heel or underside of the foot, aggravated by running, jumping, or the first steps in the morning.
- Sever’s disease and Iselin’s disease: growth-plate pain in the heel (Sever’s) or outer midfoot (Iselin’s), especially in active, rapidly growing players.
Other physical issues to watch for
- Acute sprains and strains that become chronic
- Repeated ankle sprains can leave players with ongoing instability and pain if rehab and strength work are rushed or skipped.
- Muscle strains in the groin, hamstrings, and hip flexors may recur if flexibility, strength imbalances, and training loads are not addressed.
- Growth-related coordination changes
- During rapid growth spurts, many kids become temporarily less coordinated and more injury-prone because their “new body” feels unfamiliar.
- This is a window for parents and coaches to be patient with performance and especially mindful of training load and recovery.
- Overtraining, fatigue, and burnout
- The American Academy of Pediatrics warns that intense, year-round training and early single-sport specialization increase the risk of overuse injury, fatigue, and burnout.
- Warning signs include ongoing tiredness, irritability, declining performance, frequent “nagging” pains, and a child who seems mentally checked out or dreading practice.
Red flags vs “normal” soreness
This is one of the tough ones for parents – trying to decide when something is normal and can be expected to “take care of itself”, vs when to seek professional attention. Generally, when in doubt, it’s a good idea to lean towards the latter, although it’s also true that kids are physically resilient. Some guidelines to help decide:
- Normal training soreness
- Symmetric muscle soreness in large muscle groups (both thighs or both calves) peaking a day or two after a harder session and improving with light movement.
- Discomfort that steadily improves over several days and does not limit normal walking or daily activities.
- Concerning pain (see a sports-savvy clinician)
- Pain that is sharp, localized to a specific bony spot or joint line, or present on one side only.
- Pain that persists for more than 1–2 weeks, worsens during a game or training cycle, causes limping, night pain, or affects sleep.
- Pain accompanied by swelling, locking/catching of a joint, or systemic symptoms like fever, weight loss, or general illness.
Practical prevention habits for families
- Balance and scheduling
- Aim for at least 1–2 rest days from organized sport each week and avoid playing on multiple teams with overlapping heavy schedules whenever possible.
- Be cautious with year-round single-sport specialization before puberty; variety in sports and movement patterns lowers injury risk and supports overall development.
- Training and recovery basics
- Increase training loads gradually (no big jumps in weekly volume), allow recovery after tournaments, and adjust for hard surfaces, heat, and travel.
- Encourage good sleep, regular meals and hydration, and age-appropriate strength work for the hips, core, and legs to support joints and growth plates.
- Equipment and field conditions
- Make sure boots fit current foot size, studs match the surface, and worn-out shoes or dangerous fields (holes, uneven areas) are addressed.
- Simple extras like shin guards and, when appropriate, ankle braces or tape can reduce certain injury risks when advised by a clinician.
- Communication culture
- Encourage kids to speak up early about pain instead of hiding it to stay on the field; praise honesty about their bodies as a sign of maturity, not weakness.
- Work with coaches to normalize smart rest, modified sessions, and return-to-play plans rather than the old “play through it” mindset.
